In the United States, there are approximately a million people that suffer from Parkinson’s. Parkinson’s is a Degenerative Neurological disorder that progresses over time – from mild to late stages, this disease causes increased symptoms and difficulties not only for the patient, but also for family members.
Caring for someone with Parkinson’s is not easy. It requires:
- A LOT of attention to detail and huge amounts of patience,
- An in-depth understanding of Parkinson’s symptoms, and coordinated, consistent care between family members and professional caregivers
- A recognition of the importance of medication timing, and the ability to provide systematic care support for key activities of daily life on an ongoing, consistent basis.
When you care for someone with Parkinson’s, being organized and planful is paramount to reduce stress for them and you. Each patient’s journey with Parkinson’s is different, therefore the care approach also varies – this makes it necessary to personalize care plans and caregivers to have a sustainable in-home care plan for long-term success.
With our deep experience in caring for Parkinson’s patients, this article provides you useful tips below to take care of your loved one in your home.
Parkinson’s In-Home Care and personalized care plan
Professional in-home care is your best option for long-term success in managing the progression of Parkinson’s for your loved one and balance your life accordingly.
Develop a personalized care plan according to the person’s condition (including proper diet, exercise, sleep, medications) and appoint a suitable caregiver team to help your loved one’s care per this personalized care plan.
Home Safety Precautions for Parkinson’s disease
One of the most common symptoms of Parkinson’s is mobility problems – therefore, home safety and accessibility come first. Here is a basic checklist to minimize their fall risk:
1- Flooring
- Removing rugs and any other obstacle can minimize the fall risk.
- Slip-resistance floor wax should be used to clean vinyl, hardwood, tiled floors.
- Do provide some extra space for stretching or daily exercising.
- Electrical cords must be tucked away.
2- Lightning
- All the light switches must be in your loved one’s reach.
- Install night lights.
3- Furniture Arrangements
- Furniture should be stable and accessible in their homes
- Must be placed at a distance of at least 5.5 feet.
- Install handrails for stairs.
- Clear the walkways from any decorative object like floor vases, glass objects
4- Kitchen Modifications
- Switch small knobs with some large handles or pulls.
- Items must be stored between waist and chest level.
5- Bathroom Adjustments
- Install grab bars beside toilets, washbasins, inside and outside the tub/ shower areas
- Step-less walk-in showers are ideal. If not, use a shower chair or transfer bench to bathe
- To improve traction, use non-skid mats within or outside bathtubs and sink areas.
- Skip soap bars and place washing liquid bottles for an easy grip.
- Every product (toilet papers, towels, bathing /personal care items) should be kept in their easy range.
Simplify activities of daily life for a Parkinson’s patient
Many of the activities of daily life (e.g. walking, showering, changing) which we take for granted cause immense difficulty for a Parkinson’s patient. So, simplifying their daily chores will be an important task. Fortunately, you can take care of your loved one and maintain their quality of life at home with adaptations like:
1- Personal care tips
- Use assistive devices and caregiving techniques – for example, have them use an electric toothbrush and water flosser.
- Their grooming must be done by the caregiver.
2- Getting Dressed With Parkinson’s
- Do not make haste in dressing – plan and spare longer time for getting dressed.
- Go for loose clothes that can be put in or taken off more easily and comfortably.
- Replace zippers or buttons on their clothes with velcro or magnetic fasteners.
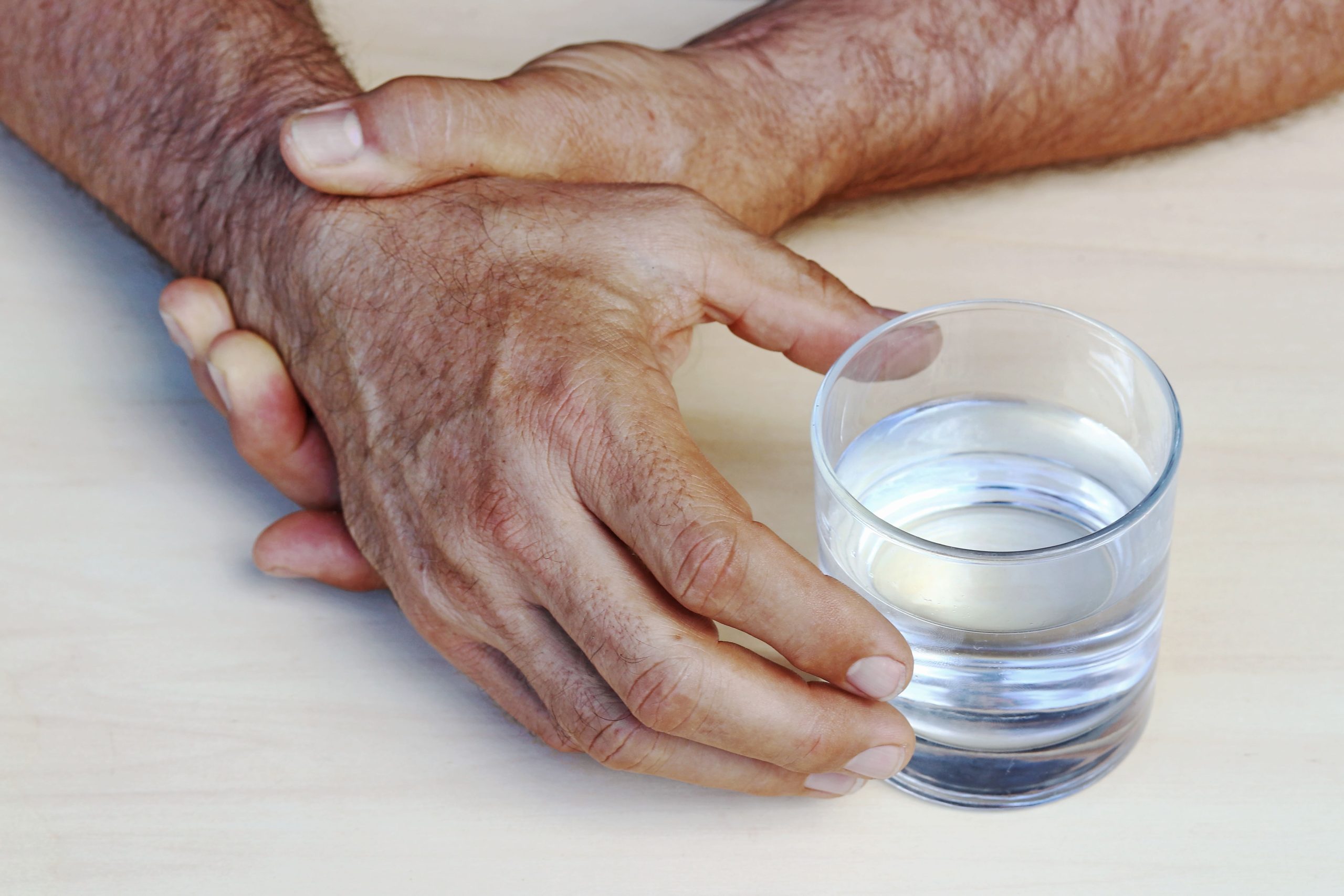
 3- Eating with Parkinson’s
3- Eating with Parkinson’s
- Utensils that are specially designed for Parkinson’s patients have padded or built-up handles and can be better used to facilitate their eating process.
- Weighted utensils and cups are more beneficial for those who find it difficult to control their motor skills.
Helping Parkinson’s Patients With Mobility
1- Freezing
Freezing is a common Parkinson’s symptom in which the person suddenly loses complete control over movement and his/her hands and legs feel rigid.
- By prompting persistently, gently, and patiently you can help them become unstuck.
- Ask them to imagine stepping over an imaginary object or line – while this sounds simple, it works very well.
- Buy a walker or rollator having a laser pointer that is specially designed for Parkinson’s
2- Exercising

Exercising can be difficult, but is VERY beneficial for the mobility of a person with Parkinson’s – physiologically, it helps the brain to use dopamine. a chemical involved in movement to help.
- Squeezing a rubber ball helps make hands and fingers more flexible.
- Daily walks and an easy exercise routine within the home helps in keeping muscles and joints more strong
- Joining yoga classes can also be helpful.
3- Inability to swallow
Difficulty or inability to swallow (dysphagia) is a disturbing symptom of Parkinson’s that affects 80% of the patients.
- Plan for 45 minutes for this task – don’t hurry them, that will only make things worse. Ensure their food is finely chopped or in purée form to facilitate eating.
- Discuss with the physician, if your loved one chokes or regurgitates food- she may recommend swallowing evaluation and make a treatment plan. If your loved one’s ability to swallow becomes worse, a caregiver MUST assist them with hand feeding.
- Help them stay hydrated throughout the day.
Planning for cognitive changes for a Parkinson’s patient
1- Watch for Hallucinations
Hallucinations (seeing or hearing something that is not there) become common in severe stages of Parkinson’s and are usually caused by an increased dopamine level (a neurotransmitter) which is not good for their mobility problems.
- Book an appointment with a neurologist.
- Try to minimize this psychotic symptom as early as possible.
2- Cognitive changes and Parkinson’s
In the middle to last stages, Parkinson’s causes changes in behavior and cognitive decline (most commonly Alzheimer’s and Dementia) in your loved ones, and it can adversely affect their mobility.
- Consult with a speech therapist if your loved one finds difficulty in communication – 90% of Parkinson’s patients have a progressive motor speech disorder.
- Be flexible and understand their condition – patiently, help them in multi-tasking, problem-solving, and planning.
- Give them more time to respond and encourage open communications.
3- Managing Sleep with Parkinson’s
Planning for REM sleep for a Parkinson’s patient is critical to slowing cognitive declines. Parkinson’s creates many challenges to getting rest and a good night’s sleep, both for the patient and the caregiver – this is triggered due to limited mobility, the effect of meds causing bad dreams or hallucinations, and frequent nighttime visits to the bathroom due to limited bladder control. Here are a few tips:
- Use different bedrooms for the patient, and other family members and caregivers.
- Choice of Bed – For the patient, consider a hospital-grade bed with a call button or alert system. Use low height beds, satin-based fabric (with less friction), light comforters, no top sheet, and a firm mattress for optimal results.
- Sleep – it doesn’t just impact the nights!
- Having loved ones and professional caregivers plan for full day coverage including nighttime shifts is very critical – this is one of the areas where most families plan poorly.
- Ensuring restful sleep for both the person with Parkinson’s and their caregivers, family members is absolutely critical – irritable and poor sleep will only exacerbate the challenges during the morning hours.
4- SKILLED THERAPIES, TREATMENT, MEDICATIONS
While there is no cure to Parkinson’s disease, there are certain therapeutic interventions that can help in minimizing its side effects by preventing muscle spasms, swallowing difficulties, loss of balance, speech problems, and correcting unsteady gait. These are some essential elements that play a vital role in a patient in-home care plan for Parkinson’s and in the related cognitive declines that are more frustrating for the affected person than their family:
- Massage therapy
- Physical and occupational therapy
- Levodopa medication
- Psychological treatments
- Dopamine agonists
- Deep brain stimulation
CONSISTENT FAMILY MEMBER & CAREGIVERS’ BEHAVIOR
In our experience, a consistent approach between family and professional caregivers is CRITICAL in managing the progressive nature of Parkinson’s and related cognitive declines. While they may sound overly simplistic, these basic principles need your full commitment to be helpful in caring for your loved one with Parkinson’s at home.
- Gain as much knowledge as you can about the disease.
- Help them feel normal.
- Get them out of the house.
- Look for any worsening symptoms.
- Be patient.
OVERALL TAKEAWAYS
Parkinson’s impacts the physical, mental, and social abilities of your loved ones. It must be their family members and professional caregivers who help ease their lives by planning ahead and resolving the issues ahead of time – We, at Care Mountain, have been providing in-home care for Parkinson’s patients for one and a half decades with our proven and personalized approach.
We are a high-quality, in-home care provider and have served over 3000+ families in DFW over the past 16 years. We have highly experienced caregivers available to support you and your loved ones’ care.
Give us a call to discuss your needs.
2022-01-18 18:33:19
Caring For a Loved One with Parkinson’s At Home – Tips For Long-Term Success!

Gagan Bhalla is the Executive Director of Care Mountain Home Health Care. For over 19 years, Care Mountain has offered dedicated expertise in senior in-home care in the Dallas Fort Worth area. Managing seven locations across Texas, Gagan has committed his life to enhancing the well-being of seniors and their families needing home health care. Through insightful articles and blogs, he shares his wealth of knowledge, empowering families to make informed decisions about home care. Trust Gagan’s experience to guide you on the path to compassionate and professional senior care.


 3- Eating with Parkinson’s
3- Eating with Parkinson’s